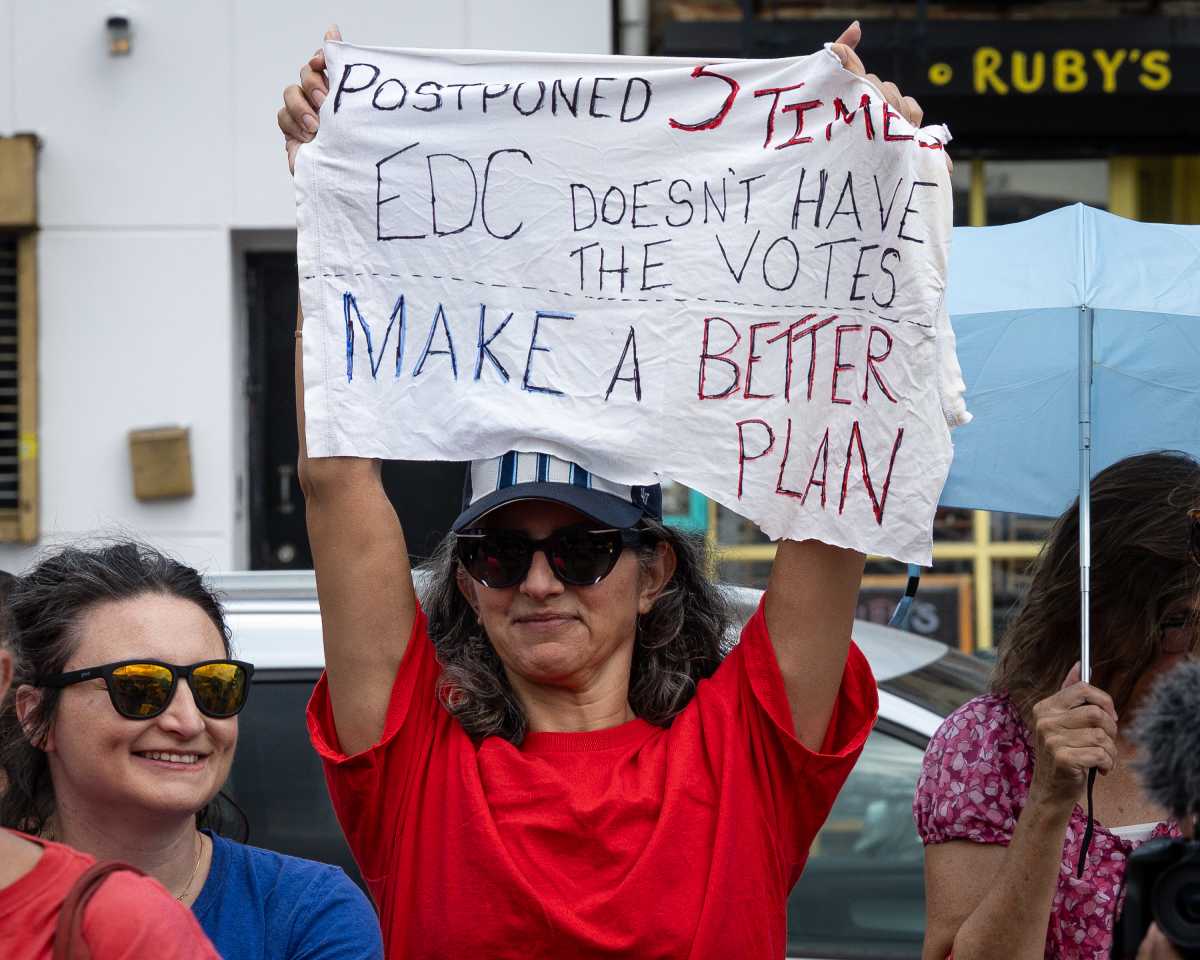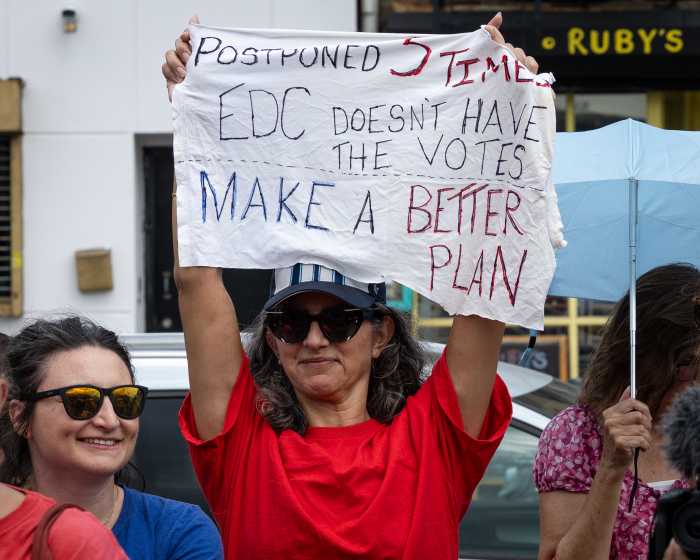Recently, Derrick Manigo started the day with a client who threatened to beat him up. Why? Probably because Manigo wouldn’t immediately give him the money to buy a toothbrush.
He’d use it to buy K2, Manigo explains.
Manigo sent the client away to cool down, like he’d done when a different client came to the outreach office barefoot and wearing only a loincloth. “You can’t come to the office like this,” he explained.
Manigo works with severely mentally ill individuals as a member of an Assertive Community Treatment team, a sort of mobile psych unit that goes to patients to deliver mental health services — both social work and often medication. Their patients are often schizophrenic, bipolar or diagnosed with borderline personality disorder and live in low-income housing, shelters or even out on the street. The long-running program, in place here since the 1990s, is one effort by city and state government to administer to some of NYC’s most vulnerable and difficult population, without resorting to jails and hospitalization. Such efforts have become more important, and sometimes more strained, as the city’s homeless population surges.
Bringing services to the homeless
On Friday, Manigo and Josiah Oborny, another member of an ACT team operated for the city by Goddard Riverside Community Center, drove around upper Manhattan tracking down some of their team’s nearly 70 clients. Manigo, a former National Guardsman from Brooklyn who had a stage acting career before coming to social work, does the driving. Oborny is a registered nurse and Peace Corps veteran responsible for medicating patients.
The two described their approach. Too often, when police officers and individuals experiencing a mental health crisis interact, the situation escalates. ACT teams, who do not travel with NYPD, try to do the opposite in their rounds, and also help their clients live comfortably in their communities. Sometimes that’s knowing that it’s best to go along with a schizophrenic patient having delusions: “yes, Obama is coming to get you in a cab, let’s wait calmly till he gets here,” Manigo says as an example. Don’t ask if the person knows what day it is.
Often, the relationship with the patients is such that they can be simple, friendly visits which build rapport over time. One client “offers me tea when I go in” says Oborny, and also did a tarot reading for him.
The pair visited a woman who, with the ACT team’s help, was able to live in her own apartment and even baby-sit her granddaughter. She refused to leave her apartment on Friday because her lock appeared to be broken, so while Oborny gave her medication, Manigo called a locksmith.
One patient who lives in a shelter wasn’t at the upper Manhattan community facility where they’d gone to find him for a routine check-in.
The patient called Manigo about an hour later.
After some small talk, Manigo asked him if he was all right. The patient was noncommittal. “I hear you’ve been sad,” Manigo said.
“Eh, what’s the difference,” the patient said. Manigo pepped him up a bit, made him agree to talk later, but if he was feeling “sad, sad,” then to call either him or anyone else from the ACT team immediately.
The man agreed.
The interaction was par for the course for the ACT team, often forced to quickly ascertain mental states and proximity to harm or self-harm. Oborny and Manigo described clients who had attempted suicide, one trying to crawl through an air conditioning vent to jump to the ground. Neither Oborny nor Manigo have lost a patient to suicide.
A model to replicate
ACT has seen drops in homelessness, hospitalizations, and harmful behavior among the nearly 3,000 clients it reaches in NYC, according to state figures. Prolonged relationships that the ACT teams provide can help avoid crises, one of the reasons programs like ACT are seen as key to accommodating mentally ill individuals to society without involving police or hospitals.
That’s something Mayor Bill de Blasio’s administration has tried with varying degrees of success. Last week, the mayor announced funding for a diversion center as an alternative to jail for the mentally ill. For ACT specifically, last year, the city increased funding for its substance abuse specialists. Gov. Andrew Cuomo is also in the process of finalizing awards for ten ACT teams devoted to the NYC shelter system.
Homeless advocates and service providers say ACT teams are an important piece of the mental health puzzle, though the teams can vary in quality and some have difficulty making sufficient contact with their patients.
This can be because the teams are “stretched too thin,” says Lindsey Davis of the Coalition for the Homeless, noting that some homeless individuals they work with have waited six to nine months to get into the program. Goddard officials say there are some 300 people on the waitlist for ACT in Manhattan. A continued housing shortage complicates ACT teams’ work if there is no housing stability in the client’s future.
But for those that get in, it can be both a health and social benefit. In the afternoon, Oborny waited for a slow elevator to visit another one of his clients, a woman who had lost touch with her family even though she was born and raised in NYC. After years of expensive and unhelpful (for her) hospital visits, she hadn’t had a serious stay in the hospital for mental issues since starting with the ACT team two years ago.
She says she gets her meals at the local senior center and made some friends there — had gotten compliments just Thursday on her new haircut. But she relied on Oborny for more long-running companionship, and said it was hard on the weekends and holidays when he wasn’t around.
“You can call anytime,” he said.
“We’ve had our ups and downs, but if he left,” the woman shook her head. “Oh no.”