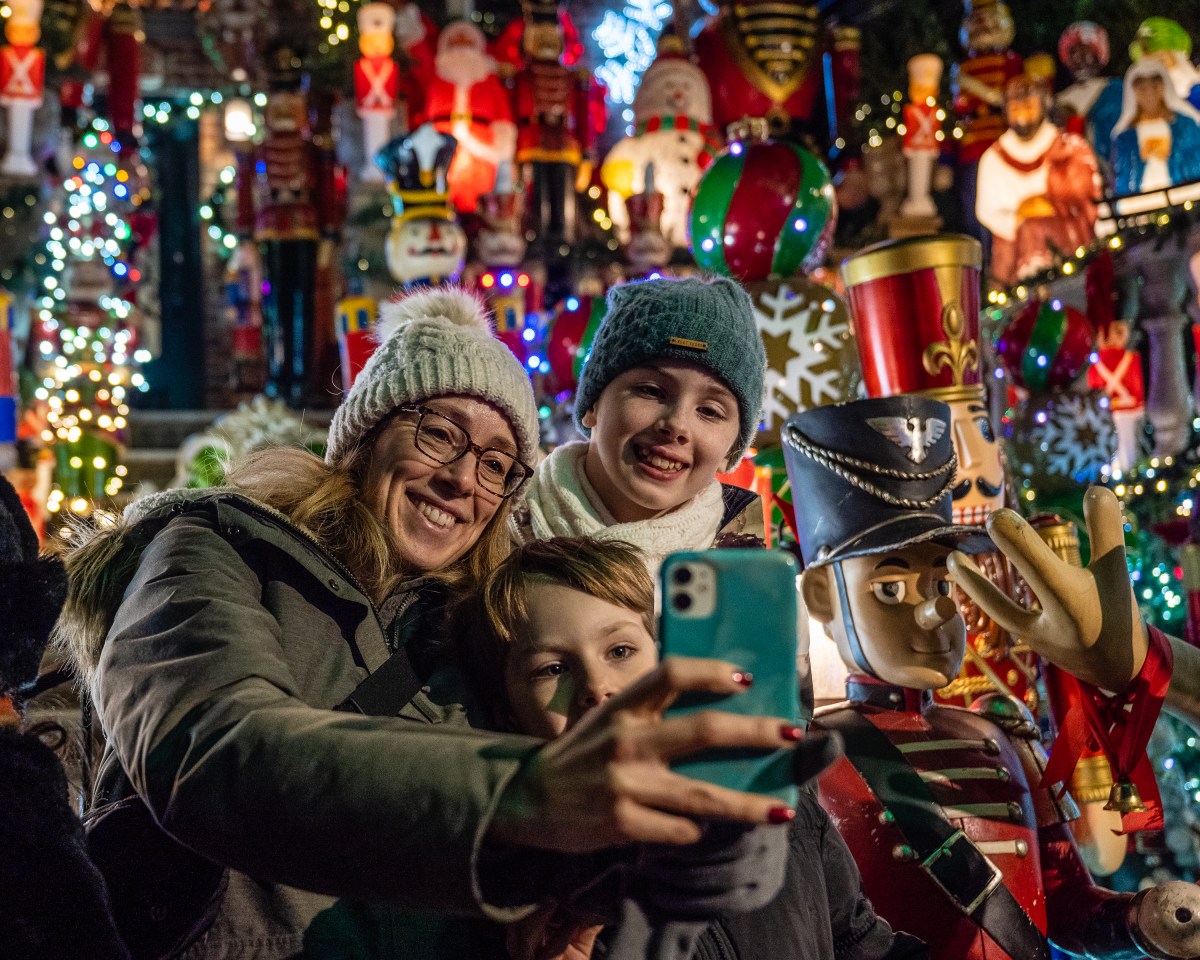
BY ALINE REYNOLDS | On 9/11, Rebecca Segarra, a seventh grader at Tribeca’s I.S. 89, saw American Airlines Flight 11 hit the North Tower of the World Trade Center from an upper-floor window in her middle school.
Shaken by the incident as a teen, Segarra said, “My anxiety just skyrocketed from there. I don’t really remember going to sleep much, ‘cause I felt like something bad was going to happen.”
Now 24, Segarra continues to suffer from insomnia, anxiety and back pains that she believes to have developed from the trauma she experienced that day. Yet, on her modest salary as a Broadway usher, she can’t afford physical or mental health treatment, and her health insurance doesn’t cover specialist care.
Segarra is also afraid of what she might be diagnosed with were she to seek care. “I don’t want them telling me something like, ‘You need treatment for this, you need treatment for that ‘cause you have this, and you can’t afford it.’ I’d just rather deal with it myself.”
Segarra is one of scores of young adults who grapple with 9/11-related health problems that interfere with their daily lives. And, though a number of them acknowledge the link between their symptoms and the terrorist attack on their neighborhood, they haven’t received federally subsidized treatment from the World Trade Center Environmental Health Center based at Bellevue Hospital Center, Gouverneur Healthcare Services and Elmhurst Hospital Center.
“I see a lot of posters about it,” Segarra said of the program, “but I’ve never looked it up or anything like that.” Asked why she hasn’t visited one of the free clinics, she replied, “I don’t really have a really good answer — I just haven’t gone.”
Currently, the W.T.C. health program is treating approximately 120 children ages 11 to 18, nearly a quarter of whom have enrolled since last fall, according to Terry Miles, director of the W.T.C. Environmental Health Center. The youths are being treated for ailments ranging from respiratory problems to post-traumatic stress disorder.
Like the adults at the center, the youths must undergo a multi-step certification process in order to be eligible for treatment. To qualify for mental health therapy, the prospective patients must answer a battery of standardized questions and, if their symptoms are judged to warrant treatment, they are assigned to individual sessions with an in-house psychologist or psychiatrist. In some cases, the youths undergo additional evaluation, are referred to mental health workers outside of the program or are enrolled in group therapy sessions within the program.
It can be a tedious process that doesn’t always get people the care they need. Bob Townley, executive director of the Manhattan Youth Downtown Community Center, said he knows of several families who have been denied treatment for 9/11-related mental health problems. “I can’t believe how many people actually can’t get mental health treatment for stuff that is clearly 9/11-related,” he said. “Usually, I’d like to think people can choose. They say they’re sick, they’re sick — especially with mental health.”
Indeed, the program’s limited number of resources hamper the amount of care that can be offered to meet the demand, said W.T.C. health program physician Joan Reibman, who accompanied Miles to Community Board 1’s Oct. 9 Youth and Education Committee meeting.
The program, she said, is “overwhelmed” with mental health issues and has therefore had to turn away people with complex, pre-existing psychological conditions. “We have many holes in the program, let me be blunt,” said Reibman. “I don’t think we will ever be able to provide pediatric psychology in-house, because we don’t have the wherewithal to do that.”
The program also lacks the funds to reimburse mental health patients for outpatient care.
The W.T.C. Environmental Health Center has also had difficulty spreading awareness of the services, Miles noted. “We’ve done focus groups where we know in the community, after all these years, no matter our efforts — the subway ads, the bus shelter ads — so many people don’t know we exist,” he said.
Youth and Education Committee chair Tricia Joyce also commented on the barriers local adults and youths have faced with respect to getting treatment at the W.T.C. clinics. “Everybody is thrilled and grateful that [the program exists],” she said, “but those have been the two things that we’ve consistently heard, the lack of mental health support and the lack of continued access and ease of process.”
While Reibman said that no additional paperwork is involved once patients are deemed eligible for treatment, she acknowledged that the program has its inconveniences.
“We certainly understand that entering the hospital, coming up to Bellevue, is a barrier — that coming to weekly sessions is a barrier,” she said, “and that we need to look at this in ways that would make it easier.”
For those who actively pursue treatment and get through the vetting process, healing can be forthcoming. Therapy sessions at Gouverneur Healthcare Services, on Madison Street in the Lower East Side, helped 24-year-old Downtown resident Charles Chawalko overcome the worst of his anxieties. A few years ago, a mental health practitioner there diagnosed him with post-traumatic stress disorder.
Chawalko recalls being generally more irritable following 9/11 and having moments of panic at music concerts and in other high-volume settings. “Sounds I wasn’t familiar with would instinctively change my heart beat,” he said, “and I would wind up getting into the cycles of paranoia and worry.”
Chawalko now has a handle on his panic attacks. He credits his progress to two years of once-a-week cognitive therapy sessions at Gouverneur, which he said fosters a comforting environment for its patients.
“I won’t say I fully mastered it, but I fully grasped a lot of the triggers I had,” he said. “The people they have are wonderful. They really try to understand you and are really good at adapting the procedures for helping you try new techniques of coping.”