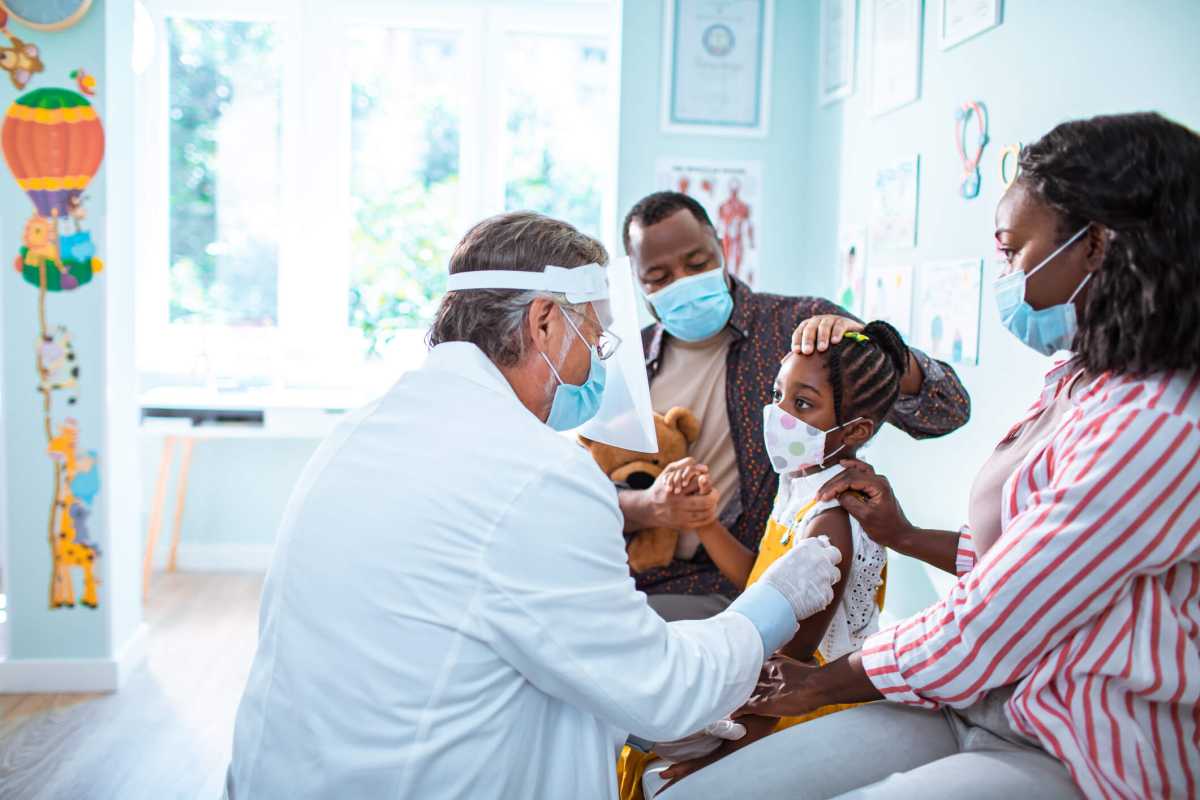
For the last two years, the COVID-19 pandemic has effectively pulled the curtain back on longstanding health inequities across the United States. Now that we are entering a tentative recovery phase, it is critical that we learn from the past two years – and, to ensure that we are ready for any future variants and that we as a city seize the opportunity to rebuild stronger, that we focus on applying a preventive care strategy.
From the beginning of the pandemic, New York City saw immense disparities in not just who got infected, but which of our friends and neighbors needed to be hospitalized, and ultimately who died. Today, out of the 39,192 people who have died from COVID in New York City, 841.6 per every 100,000 are Latino, 809.0 are Black, 449.89 are Asian, and 493.3 are white.
These trends reflect the long-standing disparities caused by language and cultural barriers, racism and discrimination, and already-disproportionate poor health.
It’s not just that a delivery worker in Jackson Heights, the school cafeteria worker from the South Bronx or the nurse from East Flatbush who had to go to work while so many had the privilege of staying home. They also likely did not have health insurance, may lack a primary care physician, access to preventative care, or other resources or information that support better health outcomes.
These are the factors that have worked against government and health care responders. And this is where a long-term preventive strategy that’s a smart use of public resources comes into play.
For five years before the pandemic, doctors and policymakers united to focus on boosting care quality while driving down costs – a formula that has consistently eluded national politicians, but that we’ve been able to get right here in New York. With the state’s support, doctors took on a challenge: how to drive down avoidable hospital visits, which cost taxpayers billions and distracted emergency room providers away from focusing on actual emergencies. The effort has been successful. In focusing on five chronic conditions that plague poor communities including obesity, hypertension, asthma, heart disease and sicknesses related to smoking, we have used a culturally competent, community-based outreach and care delivery strategy focusing on meeting patients where they are to get them in front of primary care doctors before they get sick. At SOMOS, the network I lead, that works primarily ion some of New York’s poorest neighborhoods, we have been able to raise outcomes while saving the state over $340 million dollars.
This has meant reintroducing family doctors who speak patients’ languages to neighborhoods that are otherwise health deserts or only have large, corporate hospitals where care is impersonal and intimidating – especially for immigrants – and, frequently, where staff doesn’t speak the same language as the highest-need patients. To reach patients, we have used community organizing strategies that are normally associated with political campaigns to switch emphasis off crisis management and to get them in front of doctors early. We focused on partnering with trusted neighborhood figures such as pastors, teachers and even joined up with popular entertainers to penetrate hard-to-reach communities using in-language content. And in a revolutionary formula, doctors are now being reimbursed by the state for the total health of a patient, not fee-for-service.
These non-traditional strategies have worked: by focusing on total health and on prevention, we have driven unnecessary hospital usage down by more than 25% in five years.
Back to the recovery from COVID-19.
Let’s use this moment to dramatically accelerate vaccination in all hesitant communities to prevent serious illness in case of another wave, and adopt a wraparound care strategy to do so. We must meet these New Yorkers where they are, not where we want them to be. We must partner with public housing, neighborhood media outlets and even social media influencers and well-respected local politicians, principals, pediatricians, and pastors and use them to educate and encourage. Authenticity and access are crucial.
And while any strategy must be led by doctors, an effective preventive response cannot be limited to the healthcare sector only. That’s why I am encouraged that Mayor Adams has filled his new COVID-19 task force with diverse leaders from labor, homeless services, faith, hospitality, teachers, media, representatives of businesses large and small, real estate and the disability community. Our focus will be on rebuilding a city with a stronger social fabric, long-term.
We will live with COVID-19 in some variation for the foreseeable future. But we need to prevent it from ravaging our city or bringing it to a standstill. A total-health, preventive strategy and a focus on long-term health equity can prevent future episodes from quickly becoming tragic or overly disruptive.
Dr. Ramon Tallaj is the co-chair of Mayor Adams’s COVID-19 Recovery Roundtable and Health Equity Task Force and the Chairman of SOMOS Community Care